Guidelines for research on effective treatments for kidney failure
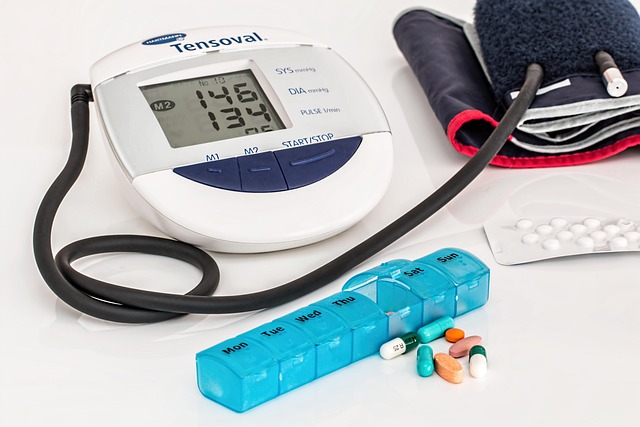
Kidney failure is a serious condition that occurs when the kidneys are no longer able to effectively filter waste products from the blood. Therefore, treatment is essential. Depending on the severity of the condition, various treatment options are available. Medications can also help manage symptoms and underlying conditions such as high blood pressure and anemia. It is important for patients to be aware of these treatment options, as this can contribute to improving their quality of life and kidney health.
Kidney failure, also known as renal failure, occurs when the kidneys lose their ability to filter waste products and excess fluids from the blood effectively. This condition can develop gradually over time or occur suddenly, requiring immediate medical attention. Research into effective treatments continues to evolve, offering patients multiple pathways to manage their condition and maintain quality of life. Understanding the available treatment options, potential complications, and lifestyle adjustments is essential for anyone affected by this serious health challenge.
Which medications are suitable for treating kidney failure?
Medication selection for kidney failure depends on the underlying cause, stage of disease, and individual patient factors. Common medications include angiotensin-converting enzyme inhibitors and angiotensin receptor blockers, which help control blood pressure and reduce protein loss in urine. Diuretics may be prescribed to manage fluid retention and swelling. Phosphate binders help control mineral imbalances that occur when kidneys cannot properly regulate phosphorus levels. Erythropoiesis-stimulating agents address anemia, a frequent complication of kidney disease. Vitamin D supplements may be necessary as failing kidneys struggle to activate this essential nutrient. Additionally, medications to manage blood sugar levels in diabetic patients and statins for cholesterol control play important roles in comprehensive kidney failure management. All medication decisions should be made in consultation with a nephrologist who can tailor treatment to individual needs.
How can patients with kidney disease slow the progression of kidney failure?
Slowing kidney disease progression requires a multifaceted approach combining medical treatment with lifestyle modifications. Maintaining strict blood pressure control is paramount, as hypertension accelerates kidney damage. Managing blood sugar levels is critical for diabetic patients, as uncontrolled diabetes is a leading cause of kidney failure. Following a kidney-friendly diet low in sodium, phosphorus, and potassium helps reduce the workload on compromised kidneys. Limiting protein intake to recommended levels prevents excessive waste accumulation while ensuring adequate nutrition. Avoiding nephrotoxic substances including certain pain medications, particularly nonsteroidal anti-inflammatory drugs, protects remaining kidney function. Regular monitoring through blood tests and urine analysis allows healthcare providers to detect changes early and adjust treatment accordingly. Maintaining a healthy weight, exercising regularly within physical limitations, and avoiding smoking all contribute to slowing disease progression. Patient education and adherence to prescribed treatment regimens remain the most significant factors in preserving kidney function for as long as possible.
How much water should a patient with kidney failure drink each day?
Fluid intake recommendations for kidney failure patients vary significantly based on disease stage, remaining kidney function, and whether the patient is receiving dialysis. In early stages of chronic kidney disease, adequate hydration supports kidney function and helps flush waste products. However, as kidney failure progresses, the kidneys lose their ability to excrete excess fluid, leading to dangerous fluid accumulation in tissues and around vital organs. Patients with advanced kidney failure or those on dialysis typically require strict fluid restrictions, often limited to 32 to 50 fluid ounces daily, including all beverages and foods with high water content like soups, fruits, and ice cream. Individual fluid allowances depend on urine output, with some patients producing little to no urine requiring more stringent restrictions. Healthcare providers calculate personalized fluid limits based on weight gain between dialysis sessions, blood pressure readings, and signs of fluid overload such as swelling or shortness of breath. Patients should never self-adjust fluid intake without medical guidance, as both dehydration and fluid overload pose serious health risks.
What are the differences in the urine of patients with kidney failure?
Urinary changes provide important diagnostic clues about kidney function and disease progression. Healthy kidneys produce clear to pale yellow urine in consistent volumes throughout the day. Patients with kidney failure often experience significant alterations in urine characteristics. Proteinuria, the presence of excessive protein in urine, causes foamy or frothy appearance and indicates damaged kidney filters. Hematuria, or blood in urine, may appear as pink, red, or cola-colored urine, suggesting kidney damage or infection. Urine volume changes dramatically as kidney failure advances, with some patients experiencing increased nighttime urination in early stages, while others develop oliguria, producing less than 400 milliliters daily, or anuria, producing virtually no urine in advanced failure. Urine may appear darker and more concentrated due to reduced kidney filtering capacity. The presence of sediment, cloudiness, or unusual odors may indicate infection or metabolic disturbances. Regular urinalysis helps healthcare providers monitor kidney function, detect complications, and adjust treatment strategies accordingly.
What are the serious side effects of medications used to treat kidney failure?
While medications are essential for managing kidney failure, they can produce significant side effects requiring careful monitoring. Angiotensin-converting enzyme inhibitors and angiotensin receptor blockers may cause dangerous potassium elevation, requiring regular blood tests and dietary adjustments. These medications can also lead to acute kidney function decline in certain situations, particularly when combined with dehydration or other medications. Diuretics may cause electrolyte imbalances including low sodium, potassium, or magnesium levels, resulting in weakness, irregular heartbeat, or confusion. Phosphate binders frequently cause gastrointestinal disturbances including constipation, nausea, and abdominal discomfort. Erythropoiesis-stimulating agents carry risks of elevated blood pressure, blood clots, and cardiovascular events when hemoglobin levels rise too quickly. Immunosuppressive medications used in transplant recipients increase infection susceptibility and may elevate cancer risk with long-term use. Some patients experience allergic reactions, ranging from mild rashes to life-threatening anaphylaxis. Drug interactions pose additional concerns as kidney failure patients often take multiple medications simultaneously. Close communication with healthcare providers about any new or worsening symptoms enables prompt intervention and medication adjustments to minimize adverse effects while maintaining therapeutic benefits.
Conclusion
Managing kidney failure effectively requires comprehensive understanding of available treatments, medications, and lifestyle modifications. Success depends on collaborative efforts between patients, families, and healthcare teams to implement evidence-based strategies that slow disease progression and maintain quality of life. Regular monitoring, adherence to prescribed treatments, and open communication with medical providers form the foundation of effective kidney failure management. As research continues advancing treatment options, patients benefit from staying informed about emerging therapies while focusing on proven strategies that protect remaining kidney function and overall health.