Skin Symptoms in Patients with Viral Liver Conditions
Viral liver conditions can manifest in unexpected ways, including various skin changes that often serve as early warning signs of underlying hepatic dysfunction. The skin, being the body's largest organ, frequently reflects internal health problems, and liver-related conditions are no exception. Understanding the connection between viral liver infections and dermatological symptoms helps patients and healthcare providers recognize these conditions earlier, leading to more timely interventions and better health outcomes.
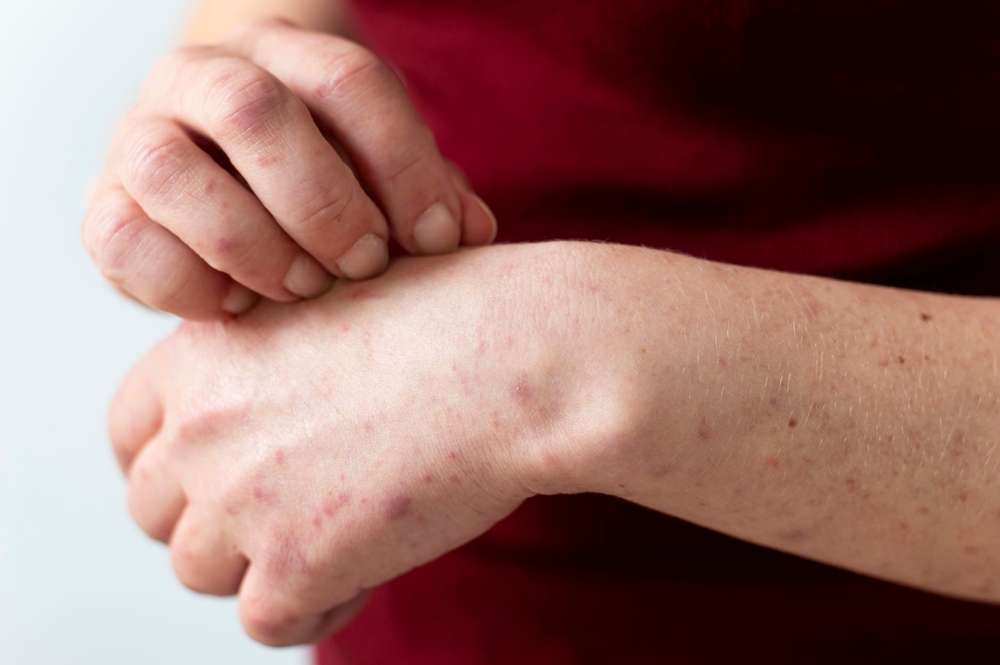
When viral liver infections occur, the body often signals distress through visible skin changes. These dermatological manifestations can appear before other symptoms become apparent, making skin observation a valuable diagnostic tool. The liver plays a crucial role in filtering toxins, producing proteins, and regulating various metabolic processes. When compromised by viral infections, these functions become impaired, leading to accumulation of substances that affect skin appearance and health.
Symptoms of Hepatitis-Related Skin Rashes
Patients with viral liver conditions commonly experience jaundice, characterized by yellowing of the skin and whites of the eyes due to bilirubin accumulation. Beyond jaundice, other skin symptoms include persistent itching without visible rash, known as pruritus, which affects a significant percentage of patients. Spider angiomas—small, red spider-like blood vessels visible on the skin surface—frequently appear on the upper body, face, and arms. Palmar erythema causes reddening of the palms, particularly at the base of the thumb and little finger. Some patients develop urticaria or hives, presenting as raised, itchy welts across various body areas. Petechiae and purpura, small red or purple spots resulting from bleeding under the skin, may also occur due to impaired clotting function.
Types of Rashes Associated with Hepatitis
Several distinct rash patterns correlate with viral liver infections. Lichen planus appears as flat-topped, purplish bumps, often affecting the wrists, ankles, and lower back. This inflammatory condition occurs more frequently in individuals with certain viral liver infections. Porphyria cutanea tarda causes skin fragility, blistering on sun-exposed areas, and increased hair growth on the face. Cryoglobulinemia-related vasculitis produces palpable purpura, typically on the lower extremities, resulting from inflammation of small blood vessels. Necrolytic acral erythema presents as well-defined, red-brown patches with scaling, primarily affecting the feet and lower legs. Polyarteritis nodosa, though rare, causes painful nodules along blood vessels and may lead to skin ulceration.
How Hepatitis Affects the Skin
The mechanisms by which viral liver conditions affect skin health are multifaceted. Impaired liver function leads to reduced bile acid excretion, causing bile salts to accumulate in the bloodstream and deposit in skin tissues, triggering intense itching. Decreased production of clotting factors results in easy bruising and bleeding manifestations. The liver’s reduced capacity to metabolize hormones causes hormonal imbalances that contribute to vascular changes like spider angiomas and palmar erythema. Immune system dysfunction associated with chronic viral liver infections can trigger autoimmune skin conditions. Additionally, direct viral effects on blood vessels and skin tissues cause inflammatory responses. The accumulation of toxins normally processed by healthy liver tissue further contributes to various dermatological symptoms.
Clinical Signs of Viral Hepatitis Rash
Healthcare providers look for specific clinical signs when evaluating potential liver-related skin manifestations. Distribution patterns often provide diagnostic clues—spider angiomas typically appear above the nipple line, while certain rashes favor the lower extremities. The temporal relationship between skin symptoms and other signs of liver dysfunction helps establish causation. Laboratory findings showing elevated liver enzymes, abnormal bilirubin levels, and positive viral markers support the diagnosis. Physical examination may reveal hepatomegaly or splenomegaly alongside skin changes. The presence of extrahepatic manifestations, including joint pain, kidney involvement, or neurological symptoms, strengthens the clinical picture. Skin biopsy findings, when performed, can show specific patterns consistent with liver-related dermatological conditions.
Differential Diagnosis for Liver-Related Rashes
Accurate diagnosis requires distinguishing liver-related skin symptoms from other dermatological conditions. Jaundice must be differentiated from carotenemia, which causes yellowing from excessive beta-carotene consumption but spares the sclera. Pruritus associated with liver disease differs from that caused by primary skin conditions, allergic reactions, or kidney disease. Spider angiomas can resemble other vascular lesions but blanch with pressure and refill from the center. Lichen planus related to viral liver infections must be distinguished from idiopathic lichen planus or drug-induced variants. Vasculitic rashes require evaluation to exclude other systemic causes of vasculitis. Comprehensive assessment includes detailed medical history, physical examination, laboratory testing including liver function tests and viral serologies, and sometimes skin biopsy. Imaging studies may be necessary to evaluate liver structure and rule out other hepatic pathologies.
Managing Skin Symptoms and Seeking Care
Patients experiencing unexplained skin changes, particularly when accompanied by fatigue, abdominal discomfort, or changes in urine or stool color, should seek medical evaluation. Early recognition of skin manifestations can lead to earlier diagnosis of underlying viral liver conditions. Management approaches focus on treating the underlying liver infection while addressing symptomatic skin concerns. Antiviral therapies targeting the specific virus can lead to resolution of many skin symptoms. Symptomatic treatments for itching include antihistamines, moisturizers, and sometimes medications that bind bile acids. Avoiding alcohol and hepatotoxic substances supports liver recovery. Regular monitoring through follow-up appointments allows healthcare providers to assess treatment response and adjust management strategies. Patient education about recognizing warning signs and maintaining liver health plays a crucial role in long-term outcomes.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.