Understanding Halitosis and Oral Care Options
Bad breath can feel embarrassing, but it is often a manageable oral health issue rather than a personal failing. Halitosis has many causes, from bacteria on the tongue to dry mouth and gum disease. Understanding what triggers it and how it is evaluated can help you choose practical, evidence-based care steps.
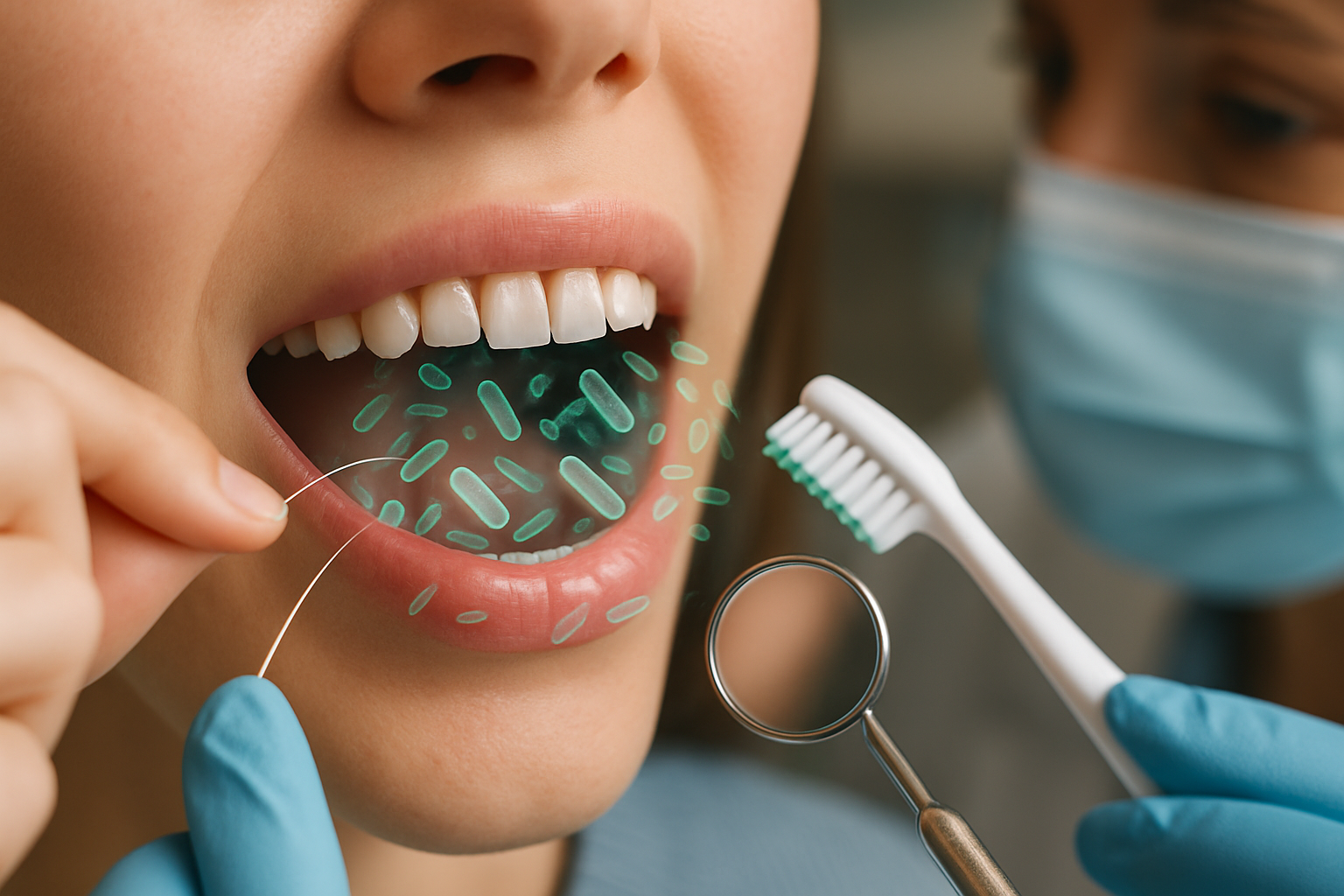
Halitosis is more than a “morning breath” nuisance—it can signal how well the mouth’s natural cleaning systems are working and whether oral bacteria are thriving. For many people in the United States, the most effective next step is not masking odor, but identifying the source (tongue, gums, teeth, or dry mouth) and addressing it with consistent oral care and professional input when needed.
This article is for informational purposes only and should not be considered medical advice. Please consult a qualified healthcare professional for personalized guidance and treatment.
Common causes of halitosis and oral health factors
Most persistent bad breath originates in the mouth. Odor-causing bacteria break down proteins and release volatile sulfur compounds, especially in low-oxygen areas such as between teeth, under the gumline, and on the back of the tongue. A coated tongue is a frequent contributor because its surface can trap food debris, shed cells, and bacteria.
Gum disease is another common driver. Gingivitis (inflamed gums that may bleed) and periodontitis (deeper infection with bone and tissue loss) can create pockets where bacteria and debris accumulate, producing a chronic odor. Untreated cavities, failing dental restorations, and trapped food between teeth can also contribute.
Dry mouth (xerostomia) often amplifies halitosis because saliva normally rinses away debris and helps control bacterial growth. Dry mouth may be related to dehydration, mouth breathing, sleep habits, certain medications (such as some antidepressants, antihistamines, and blood pressure drugs), and conditions that reduce saliva. Diet and lifestyle factors matter too: tobacco use, frequent alcohol intake, and strongly scented foods can worsen odor, while very low-carbohydrate diets may cause a distinct breath odor due to ketosis.
How halitosis is diagnosed by dental professionals
A dental evaluation typically begins with a medical and dental history focused on timing (morning-only versus all day), triggers (certain foods, fasting, medication changes), and associated symptoms (dry mouth, bleeding gums, reflux symptoms, nasal congestion). A clinician may ask about oral hygiene routines, including brushing frequency, flossing or interdental cleaning, and whether the tongue is cleaned.
The clinical exam usually includes checking for gum inflammation and pocketing, plaque and tartar buildup, cavities, cracked teeth, ill-fitting crowns or bridges, and signs of oral infection. Because the tongue is a common source, many dental professionals will assess tongue coating and recommend specific cleaning techniques.
In some cases, practitioners use organoleptic assessment (a trained smell evaluation) as a practical method, along with targeted measurements such as periodontal probing. Specialized devices that measure volatile sulfur compounds exist in some clinics, but a thorough exam and history are often enough to identify likely causes. If the mouth appears healthy and halitosis persists, the dental team may suggest medical evaluation for less common contributors such as chronic sinus issues, reflux, or other systemic factors.
Treatment approaches for persistent bad breath
Treatment usually starts with controlling bacterial buildup and addressing inflammation. For many people, improving technique and consistency is more effective than adding many new products. Brushing twice daily with fluoride toothpaste, cleaning between teeth daily (floss or interdental brushes), and gently cleaning the tongue can reduce odor sources that brushing alone may miss.
Professional care is important when gum disease or tartar is present because hardened deposits cannot be removed with home tools. A dental cleaning and, when indicated, periodontal therapy can reduce bacterial load and gum pocket depth, which can meaningfully change breath over time. Repairing cavities, replacing defective restorations, and treating oral infections also removes sites where odor-causing bacteria persist.
Mouthrinses can be helpful as a supporting tool, but they work differently depending on ingredients. Some rinses reduce bacteria temporarily, some neutralize odor compounds, and some include fluoride for cavity prevention. Overuse of harsh or highly drying products may worsen dry mouth for certain people, so it can help to discuss options with a dental professional—especially if you already struggle with dryness, irritation, or sensitivity.
If dry mouth is a key factor, strategies may include improving hydration, limiting alcohol-based rinses, addressing mouth breathing when possible, and reviewing medications with a clinician if symptoms began after a new prescription. Sugar-free gum (particularly with xylitol) may stimulate saliva for some individuals, but it is not a substitute for treating gum disease or decay.
Long term oral care strategies for halitosis
Long-term control is usually about building a routine that reduces plaque consistently and supports a healthier oral environment. Many people benefit from setting a simple baseline: brush along the gumline for a full two minutes, clean between teeth once daily, and add tongue cleaning as a standard step rather than an occasional fix.
Regular dental visits help catch problems early, including gum inflammation, hidden decay, and failing restorations that can trap debris. If you have a history of periodontitis, maintenance intervals may be shorter than for someone without gum disease, because bacteria can recolonize periodontal pockets and reignite inflammation.
Lifestyle habits often determine whether results stick. Staying hydrated, limiting tobacco, and moderating alcohol can reduce dryness and bacterial overgrowth. If certain foods consistently trigger odor, rinsing with water after meals and cleaning between teeth later in the day may help. For people who snore or breathe through the mouth at night, discussing nasal congestion or sleep-related concerns with a clinician may be relevant, since nightly dryness can undermine otherwise good hygiene.
Finally, consider tracking patterns for a few weeks: when odor is worst, what oral care steps were skipped, and whether dry mouth symptoms are present. That record can make dental appointments more productive and help distinguish routine oral causes from problems that might require medical evaluation.
Persistent halitosis is often treatable once the main source is identified—commonly tongue coating, gum disease, dry mouth, or trapped debris from dental issues. A combination of consistent daily cleaning, targeted products when appropriate, and professional assessment for underlying dental conditions provides the most reliable path to longer-lasting improvement.